
Document 1
IN CONFIDENCE
Briefing for decision
Digital access for rural communities
Date due to MO: 8 May 2025
Action required by:
<N/A>
Security level:
IN CONFIDENCE
Reference:
H2025064699
To:
Hon Matt Doocey, Associate Minister of Health
Consulted:
Health New Zealand ☒ Ministry of Social Development ☒
1982
Ministry for Primary Industries ☒ Ministry of Business, Innovation and
Employment ☒
Act
Proactive release: This
title is proposed by the Ministry of Health for proactive release: ☒
Information
Contact for telephone discussion
Name
Position
Telephone
Official
Caleb Johnstone
Acting Group Manager, Primary, Family
s 9(2)(a)
and Community Health Policy
the
Sam King
Manager, Health System Stewardship
under
Minister’s office to complete:
☐ Approved
☐ Decline
☐ Overtaken by events
Released
☐ Needs change
☐ Seen
☐ See Minister’s Notes
☐ Withdrawn
Comment:
IN CONFIDENCE

1982
Act
Information
Official
the
under
Released
Document 1
IN CONFIDENCE
s 9(2)(f)(iv)
8.
Recommendations
s 9(2)(f)(iv)
1982
Act
Information
Official
the
under
Released
Caleb Johnstone
Hon Matt Doocey
Acting Group Manager, Primary, Family and
Community Health Policy
Associate Minister of Health
Strategy, Policy and Legislation
Date:
Date: 8 May 2025
Briefing: H2025064699
2
IN CONFIDENCE
Document 1
IN CONFIDENCE
Digital access for rural communities
Background and context
Current rural barriers to accessing health care
1.
Rural communities face chal enges in accessing health services. Digital access can
improve health by providing consultations with medical professionals in primary care,
urgent care and unplanned care.
2.
Expanding digital options is a key shift needed to improve rural health outcomes.
However, digital access remains a significant barrier for rural communities in accessing
online health services. Enhancing digital access will be critical in enabling rural
communities to access a range of health care services.
1982
3.
The Ministry currently has work underway to support healthcare access for al New
Zealanders. The primary care work programme has initiatives such as 24/7 digital
Act
services, urgent care and unplanned care that require digital infrastructure to be
accessed. The Ministry would need to work out how these initiatives would work along
side digital access barriers experienced by rural communities.
Rural health actions and strategic drivers
4.
As part of your request for possible actions related to your associate health delegations,
we identified a possible opportunity to increase access to online heal
Information th services. This
work is part of your current associate health work programme for rural health as action
3.4.2, where the Ministry is working cross-government to improve digital access for rural
communities (HNZ00050253).
5.
There are opportunities to improve health access
Official for rural communities through
increased digital access. Options that improve digital access align with current
government priorities for improving a
the ccess to health.
a.
The Government Policy Statement on Health 2024–2027 (GPS): Access is a
priority area in the GPS, where ‘every person, regardless of where they live in New
Zealand, has equitable acc
under ess to the health care and services they need’. Increasing
digital options, through telehealth or online resources to support mental wellbeing,
wil increase access if people have reliable digital access within their homes or
communities.
b.
Rural Health Strategy: Priority 3, services are available closer to home for rural
communities, includes digital services so individuals have access in their homes or
Released
communities. Where services are not available rural y, Priority 4 supports rural
communities to access services at a distance, which can include supports for digital
access such as enabling video telehealth consults.
c.
Transforming primary care: The Primary Care Tactical Action Plan aligns with the
expectations and priority areas set out in the GPS, including for mental health and
addiction. The Tactical Action Plan outlines actions that wil be the building blocks of
improvement to primary care delivery, including 24/7 digital access to primary care.
d.
Ka Ora Telecare: Ka Ora is an after-hours video and over-the-phone health service
helping to support the health of people in rural communities. Telehealth is used to
Briefing: H2025064699
3
IN CONFIDENCE
Document 1
IN CONFIDENCE
prevent delayed or avoided healthcare due to access barriers faced by rural
communities.
Digital options to improve access to health services
6.
Expanding digital health options that improve access to health services are part of work
Health New Zealand (Health NZ) will consider in progressing expectations from the GPS.
Options include video telehealth, online tools for mental wellbeing and remote patient
monitoring, such as hospital at home. This briefing looks at supporting digital access to
be able to take up digital health options.
Current levels of digital access
7.
There are digital access issues in rural communities that are not reflected in urban
settings. Urban communities general y have fibre options, better mobile data and easier
access to publicly available internet services provided at community hubs. Fibre options
1982
for digital access provides many New Zealanders with a reliable connection, high levels
of internet access and speed, and minimal interference with environmental factors such
Act
as weather.
8.
Rural communities without fibre rely on digital infrastructure that is often charged to
consumers at a higher cost and may be less reliable than fibre. For example, copper,
cellular fixed wireless, non-cellular fixed wireless, and satellite options. This contributes
to barriers for rural households to get internet access and as a result, means they have
fewer viable options for accessing health services when they are offered online.
Information
9.
Improving digital connectivity is a priority for rural communities. Rural Women New
Zealand highlighted that the lack of highspeed reliable, quality, and affordable
telecommunication services in rural areas exacerbates inequity in health outcomes for
rural communities.
Official
10.
Overall, internet access within rural households has improved from 70% in 2013 to 81%
in 2018, and 86% in 2023. This is low
the er than in urban areas, where access is around 91%.
Within rural areas, as defined for health1, there are larger areas with fibre and those close
to urban communities with internet access comparable to urban areas. However, there
are stil higher gaps for some rural communities. For example, the Great Barrier Local
under
Board Area has the lowest rate of household internet access2, at 66%, with other rural
communities in the Far North, Opotiki, Wairoa and Ruapehu having rates under 75%.
11.
In 2023, there were around 300,000 people living in rural areas with no or very low fibre
options:
a. Over one third of connections in the most remote rural areas had copper
Released
connections
1 Health agencies use the Geographic Classification of Health for defining rural and urban areas within New Zealand. This
relates to the size of the community and its distance to main urban centres and the higher-level health services available.
When rural areas are referred to throughout this report, it relates to this definition of rural, not telecommunication
companies’ definition of rural as where fibre is not available.
2
The National Infrastructure Funding and Financing Company are looking at building a new cell tower in the Great barrier
Local Board Area. This may help improve coverage in the area. Negotiations are ongoing.
Briefing: H2025064699
4
IN CONFIDENCE
Document 1
IN CONFIDENCE
b. Around one in five rural households, that are close to urban areas or larger rural
towns, had copper connections
c. For the main urban centres, the share of copper connections is around 5%.
12.
Household connections in rural areas comprise just over 50% of total satellite
connections. In 2023, 1 in 20 households in rural areas had a satellite connection for
their digital access.
Technology market changes and mobile data
13.
New Zealanders are general y increasing their access to the internet and digital options
through their phone’s mobile network, including for apps related to health or for
telehealth video cal s.
14.
Mobile network coverage for data can be limited or unreliable in some rural
communities. Currently, One New Zealand (One NZ), a telecommunications company
1982
has introduced a satel ite option that enables those out of traditional cell-tower
coverage to text anywhere in New Zealand. The ability of rural communities with poorer
Act
network connections to use mobile data could improve over time as more partnerships
develop between mobile providers and satellite options. Development in satellite
options and further technology advancements shows to promise to provide capacity for
audio and video. This would be supported by satel ite options through mobile phones,
allowing overall digital access to improve for rural communities.
15.
Mobile network changes that lead to improvements in digital access for rural
Information
communities could also improve health outcomes for patients. Mobile digital access
supports wider access to digital health options (outlined in paragraph 3 above) and
growing health technology that is digital y connected, such as wearable devices.
Wearable devices, especial y with mobile data, increase patient autonomy in managing
their health conditions at home. Wearable devices
Official provide options for clinical oversight
and support proactive management for individuals with chronic health conditions.
the
16.
Improved mobile coverage would also mean more people in rural communities are able
to benefit from the Government’s Zero Data initiative. Within health, the Zero Data
initiative reduces financial barriers to digital health services by providing free access to
key health sector websites on mobile networks, if accessed from the Zero Data website.
under
Opportunities for increased digital access
Financial barriers have replaced technological barriers 17.
The barriers to digital access in rural communities are now more financial than
Released
technological due to expanded technological options and changes to the corresponding
market.
18.
Previously, the lack of infrastructure available was the main barrier to digital access for
rural communities. This was because of the difficulty, inability, and cost to install
technology in rural areas. At this time, government mainly focused on improving digital
infrastructure in rural communities to improve their digital access.
19.
Since 2010, government has invested more than $770 mil ion into rural connectivity.
Many rural communities have benefited from rural broadband infrastructure investment.
Briefing: H2025064699
5
IN CONFIDENCE
Document 1
IN CONFIDENCE
For example, from 2018 to 2023, the household internet access rates in the Chatham
islands grew from 65% to 87% after investment in digital infrastructure.
20.
Low earth orbit (LEO) satellites, such as from Starlink, a telecommunications company
(available to residential houses since 2021), provide New Zealanders with high-speed,
reliable internet to people with no, intermittent or slower options in rural areas.
However, when Starlink plans are compared to standard offers for fibre options, Starlink
currently has higher monthly costs ($79 for low usage plan only available in limited areas
compared to $65 for low fibre usage plan, and $159 for high-speed plan compared to
$96 for high-speed fibre plan), and initial cost barrier of installation ($449 for Starlink
compared to $213.95 for fibre plan if a modem is required, as at April 2025), which
create financial barriers to accessibility.
21.
While installation costs have fallen from their initial market offer, significant further
reductions are unlikely to change until competition enters the market to put downward
pressure on prices. Even if market pressures reduce costs for rural communities, fina
1982ncial
barriers wil remain for some groups. There are currently no other LEO satellite options in
the residential market. However, new providers and more options for increased
Act
connectivity in partnerships with existing mobile providers are expected.
Current Government-led connectivity options that support rural communities
22.
The Ministry for Business, Innovation and Employment (MBIE) and the Ministry for Social
Development (MSD) are involved in supporting digital connectivity for rural
communities.
Information
23.
Community facilities with digital access can provide valuable and effective options to
support digital access. In comparison to people in urban areas that have financial
barriers, rural people are general y less able to rely on community-based options, such
as schools or libraries for digital access, and these facilities may also be a significant
Official
distance from their homes.
24.
MBIE and MSD currently fund comm
the unity facilities that provide digital inclusion support
options for rural communities:
a. Heartland Services (Heartlands) – supports rural and isolated communities to
access government and non-government services. While Heartlands mainly seeks
under
to provide advice and a physical space or hub so people can access services face
to face, it also provides digital access to the community. MSD currently funds
Heartlands in 39 communities across New Zealand.
b. Marae Digital Connectivity Programme (MDC) – the MDC supports internet access
for marae, al owing whānau and hapū to undertake economic activity and enhance
Released
their digital capabilities. MBIE, with the National Infrastructure Funding and
Financing Company (formerly Crown Infrastructure Partners), fund
telecommunications partners to provide grant-funding for the MDC. A total of
$21.9 mil ion had been al ocated to the MDC from when it commenced in 2019 to
June 2024. A scaled extension of the MDC until 30 June 2027 has been funded
through the reprioritisation of a $5 million forecast underspend of the Remote
Users Scheme, in addition to $1.2 million of baseline funding. As of December
2024, 667 marae across rural and urban areas received support from the MDC.
Briefing: H2025064699
6
IN CONFIDENCE
Document 1
IN CONFIDENCE
c. Regional Digital Hubs – provided key digital services and equipment to help rural
communities stay connected to the rest of the country. MBIE rol ed out regional
development funding for these hubs in 2019. There are 16 regional development
hubs that have benefitted from this initiative in Northland, Bay of Plenty, East
Coast/Tairāwhiti, Hawke’s Bay, Manawatū-Whanganui, and the West Coast. The
hubs received startup funding from the Provincial Growth Fund (PGF) but do not
receive ongoing government funding as PGF programmes are ending and
contracts with the hubs have ended or are ending in the next year.
25.
These programmes are the existing government-funded community-based support that
provide internet access for rural communities. There may be other local initiatives that
provide community hubs with digital access.
26.
MBIE, through the National Infrastructure Funding and Financing Company, previously
funded the Remote Users Scheme until the end of 2024 to provide one-off $2,000 grants
to those outside of terrestrial broadband coverage with limited connection options.
1982
Most of this funding went towards purchasing Starlink kits.
27.
MBIE’s focus is on telecommunications infrastructure, not digital inclusion a
Act nd MBIE-led
programmes have already ended or will end by 2027. In comparison, Heartlands receives
ongoing funding from MSD. This should be noted when considering opportunities for
increasing digital inclusion.
28.
The health sector also support digital access for health purposes. This includes funding
some telehealth booths for consults with specialists in some rural areas, such as Hawera,
to reduce the need to travel into urban hospitals, or initiatives in som
Information e areas where
patients are supported to access appointments from home. People, such as paramedics
or community workers, bring digital capability and medical specific equipment for
monitoring. These only serve specific appointments for planned care.
29.
Under Heartland service guidelines, there is an ex
Official pectation that al Heartland facilities
have the capacity to support people to access telehealth services. This includes physical
infrastructure to provide a safe, secur
the e, and confidential space, digital infrastructure such
as Wi-Fi, computers and printers, and staff such as coordinators and interpreters who are
able to support individuals during their telehealth consultations. Support for these
services is dependent on the needs of the community.
under
s 9(2)(f)(iv)
Released
Briefing: H2025064699
7
IN CONFIDENCE
Document 1
IN CONFIDENCE
s 9(2)(f)(iv)
34.
Existing community hubs with digital access have been set up for a range of purposes.
They are not able to be informed by a current assessment of digital access gaps and
needs with current technology options. An assessment of where there are the most
digital access gaps and a range of community facilities considered, could see
government make more effective funding decisions to boost digital access. 1982
35.
The provisional assessment of digital access needs for rural communities is outlined in
Appendix 2. The map shows the geographic rural communities with poor access, and
those with higher needs for digital options, due to distance to services. The m
Act ap
considers household internet access, connection type and distance to main centres,
where there is less alternative digital access options and more benefits to patients from
less travel.
36.
The main areas with poor access and higher needs are in Kaipara, Opotiki, South
Waikato, Ōtorohanga, South Taranaki, Waimate, Westland and Southland. Some of these
areas, such as Opotiki, have existing government-funded community a
Information ccess, such as
from the MDC and Heartlands.
s 9(2)(f)(iv)
Official
the
under
Released
Briefing: H2025064699
8
IN CONFIDENCE
Document 1
IN CONFIDENCE
s 9(2)(f)(iv)
1982
Act
Information
Official
the
under
Released
Briefing: H2025064699
9
IN CONFIDENCE
Document 1
IN CONFIDENCE
s 9(2)(f)(iv)
1982
Act
Information
Official
the
under
Released
Briefing: H2025064699
10
IN CONFIDENCE
Document 1
IN CONFIDENCE
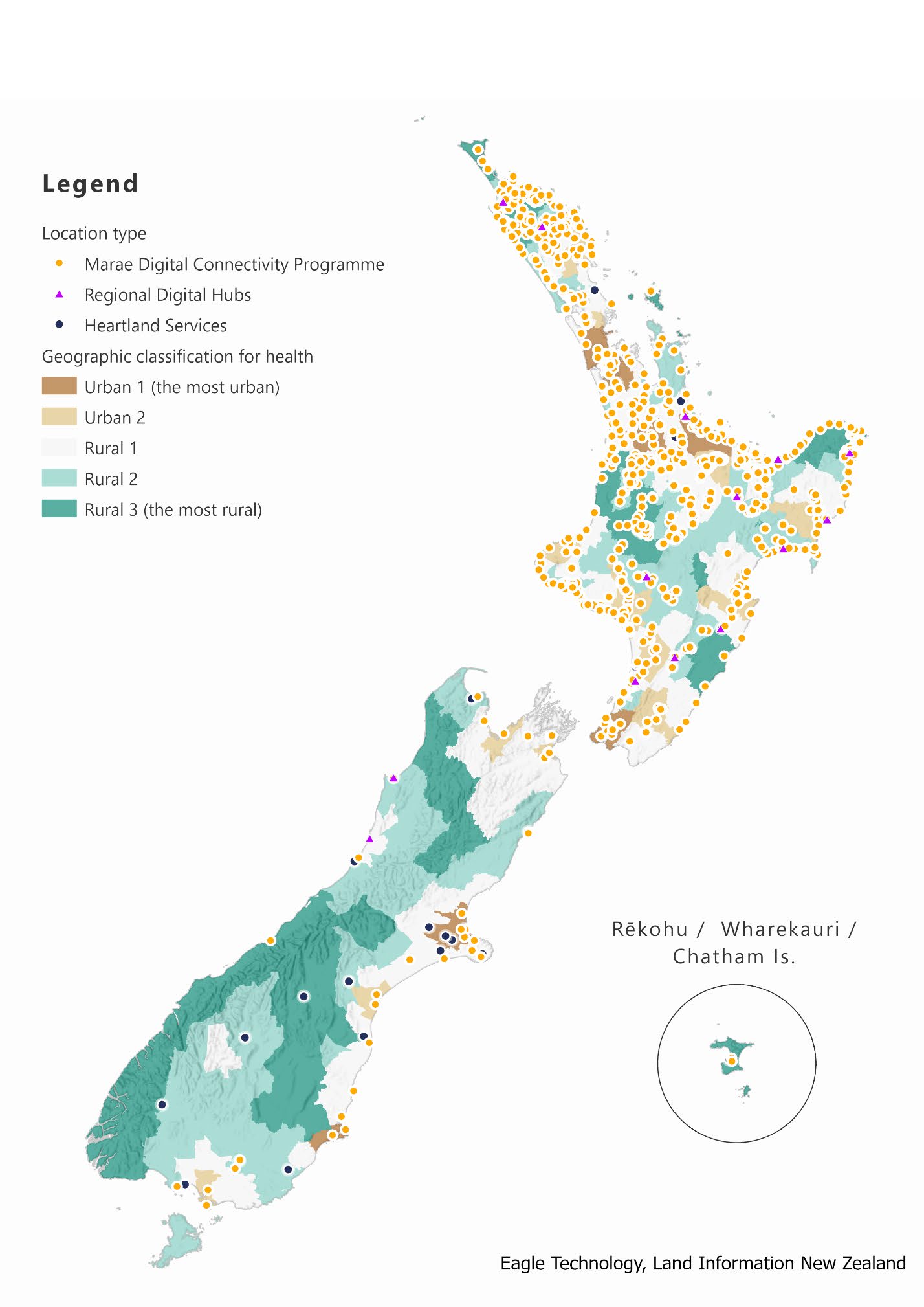
Appendix 1: Map of Government-funded Community hubs that have in digital access
(Heartlands services, regional digital hubs, and the Marae digital connectivity programme)
1982
Act
Information
Official
the
under
Released
Briefing: H2025064699
11
IN CONFIDENCE
Document 1
IN CONFIDENCE
Appendix 2: Assessment of digital access gaps in rural communities
We have undertaken an initial assessment of relative needs and digital access gaps within rural
areas. The criteria in assessing this aims to highlight rural areas with the highest need for digital
access to outline where digital gaps are for rural communities geographical y, and as the basis for
informing priority areas for any expansion to community hubs.
To target our areas of focus to where there is need, we have excluded areas that are in, or close to,
main urban centre or provincial cities. These areas have closer access to key services, including
health, and general y have fibre options and more community facility options.
The factors we have used in the assessment of rural geographic areas include areas with:
a.
with lower percent of households with internet access (any internet option)
b.
more likely to have households without any internet connections with
telecommunications providers
1982
c.
with a high percentages of copper connections (as this indicates likely to have lower
quality access in households)
Act
d.
where there has been higher growth in the use of a satellite option. This may indicate a
gap in other quality options but can also mean many households are not having
financial barriers to take it up quickly.
e.
that are a significant distance away from urban centres, requiring individuals to have
high transport times for access broader health care options, or fuller range of other
government services.
s 9(2)(f)(iv)
Information
where there are geographic gaps in community digital access options, such as marae and
Heartlands (see Appendix 1 for maps of current community hubs supports).
Category
Descriptors around
Household internet
Descriptors around need
Official
connections
access levels (2023
census)
Good access (high
Fibre 40%+; very low
Primarily non-deprived
the
fibre)
satel ite options
Average 92%
areas
Good access
(mixed
Cooper and/or sat
Mainly non-deprived
connections)
higher than fibre
under
Average 91%
areas
Mixed access (high
Fibre 40%+, with low
Majority of areas are high
fibre)
satel ite, others mixed
Average 82%
or moderately deprived
Mixed access (high
Average satellite level
Some geographically
satel ite)
for group around 30%
Average 85%
isolated areas
Mixed/poor access
Reported high levels of
(lower connections
Released
households not connected
and low fibre)
Limited fibre or satel ite
Average 87%
to internet provider
Less remote rural areas –
No, limited, fibre,
and areas are more
Poor access (less
mainly copper- growing
deprived communities, in
remote)
satel ite
Average 81%
general
No, limited, fibre,
More remote (R2 or R3);
Poor access (more
mainly copper- growing
around ¾ of areas in
remote)
satel ite
Average 80%
lowest deprivation quintile
Briefing: H2025064699
12
IN CONFIDENCE
Document 1
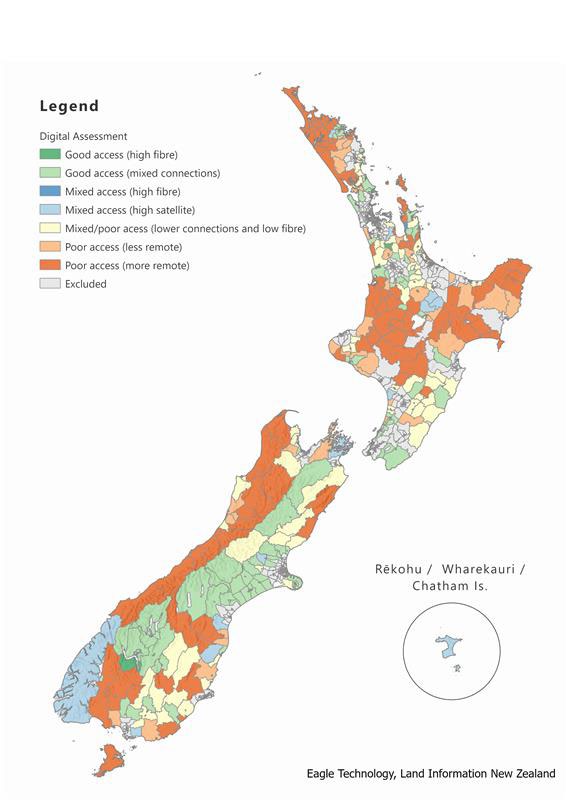
IN CONFIDENCE
Map categorising rural areas by digital access needs and digital infrastructure
1982
Act
Information
Official
the
under
Released
Briefing: H2025064699
13
IN CONFIDENCE
Document 1
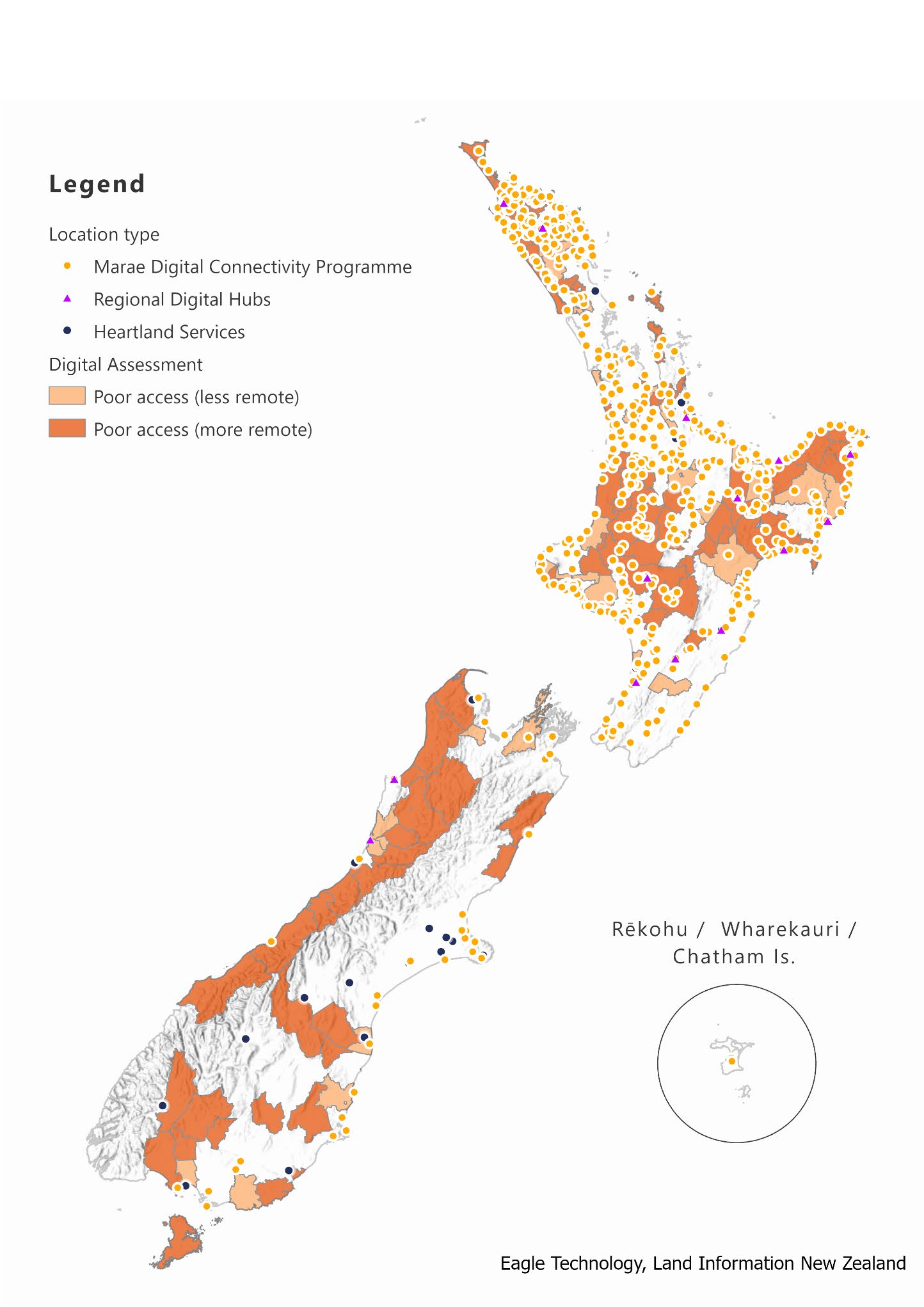
IN CONFIDENCE
Map categorising poor digital access by remote levels, and location of government-funded
digital access community hubs
1982
Act
Information
Official
the
under
Released
Briefing: H2025064699
14
IN CONFIDENCE

Document 2
IN CONFIDENCE
Excerpt from Weekly report 29 August 2024
13 Associate Ministers of Health
Out of scope
13.2 Hon Matt Doocey
13.2.1
Digital inclusion for rural communities
This is an update related to the Associate Health portfolio priorities, rural health, action 3.4.
Internet connectivity in rural areas remains a barrier to accessing health services with digital options, as wel as
other government services, education provision or online work. Expanding digital health options is an
1982
expectation in the Government Policy Statement on Health 2024 - 2027, which Health NZ wil be progressing.
However, if there are significant gaps in digital access for rural communities, this reduces the effectiveness of
Act
digital options.
Internet connectivity is often less reliable and higher cost in rural communities than in urban areas. Some
sparsely populated areas, such as the East Coast of the North Island and West Coast of the South Island, stil
have significantly lower levels of household access to the internet. Government investment in rural
infrastructure and the availability of low-earth-orbit satel ites means that availability of connectivity solutions is
now not the primary barrier for rural communities in accessing digital connectivity.
Increasing satel ite-based options (such as Starlink), provides a technological access
Information change, but the financial
barriers for affordability stil exist, while competition further develops.
The Commerce Commission’s 2023 Telecommunications Monitoring Report (published August 2024) outlines
the growth in Starlink with the fol owing key information for rural areas, where no fibre options exist:
Official
as at June 2023, there were 34,000 low-earth-orbit satel ite connections (Starlink) in rural areas, with 14%
of the rural market (expected to have continued significant growth since June 2023)
the
copper network connections are stil the most common (3.33%), but have fal en considerably
while there are cel ular network options, they often have data caps.
Having internet access at community-based sites, such as existing Ministry of Social Development (MSD)
under
Heartland services (44 sites) or Rural Digital Hubs (14 sites), established through the Provincial Growth Fund
(administered by the Ministry of Business Innovation and Employment (MBIE)), provide options for people in
communities with more limited connectivity or financial barriers. In addition, to support health access, there
are also telehealth ‘booths’ at some health facilities, and some initiatives that provide mobile and clinical
support in-home to link via telehealth to specialist care.
s 9(2)(f)(iv) Released
20
IN CONFIDENCE

1982
Act
Information
Official
the
under
Released






